Clinical pathway for healthcare dentists and software development that can diagnose osteoporosis. Researcher Joanna Golberg says there are two success factors for dental care to be able to contribute to the detection of osteoporosis.
Osteoporosis means weakening of the skeleton and can lead to bone fractures. These bone fractures cause great suffering to the patient, but are also among the most costly to healthcare. Hip fractures in particular require a long time in the hospital.
Osteoporosis
Osteoporosis is a silent disease that is first noticed in many cases in broken bones. Annually, approximately nine million osteoporosis-related fractures occur worldwide. A third of these occur in Europe, Sweden, Norway and Denmark at the top with more than 500 broken bones per 100,000 inhabitants. In addition to osteoporosis, age, and previous bone fractures or bone fractures in close relatives, certain medications and diseases as well as smoking and alcohol are risk factors for bone fractures. Osteoporosis is more common in women than in men.
Too expensive to screen high-risk patients
There is no economic justification for screening at-risk patients in healthcare for osteoporosis. The evaluation is usually done instead after the first fracture. However, previous studies have shown that there is a relationship between age-related changes in the jawbone and in other parts of the skeleton. This is where dentist Joanna Golberg believes that resources in dentistry can be used to screen for individuals at risk for osteoporosis and bone fractures.
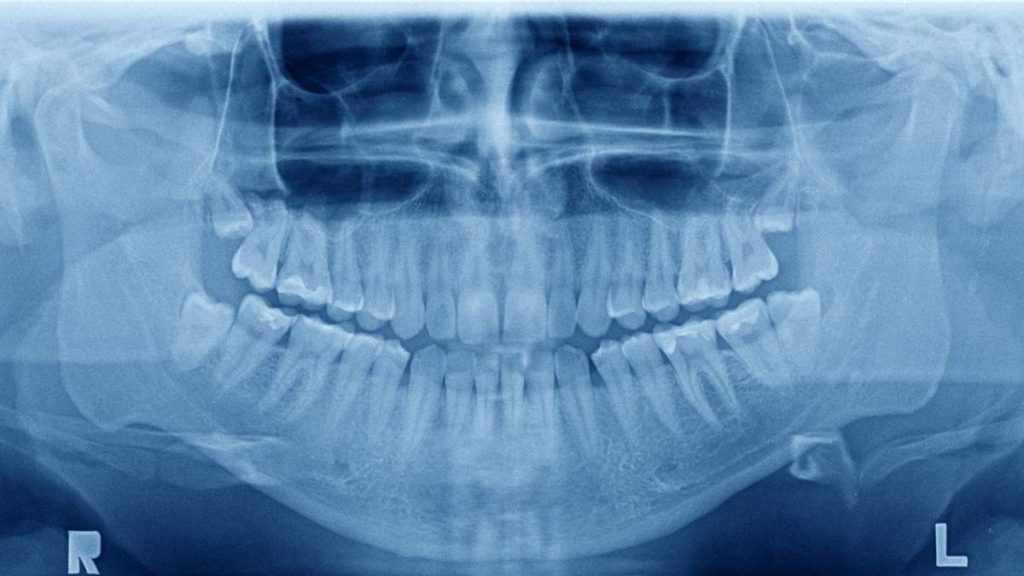
Dental and maxillofacial x-rays are done regularly, especially in Sweden where most people go to the dentist annually. These are still images and can also be used to assess osteoporosis, says Joanna Golberg, who is currently defending her thesis at Malmö University School of Dentistry.
Women at risk are willing to pay
In her dissertation, through focus group interviews, she examined the situation between dentists and at-risk patients to provide an assessment of osteoporosis to the dentist. The situation was generally positive, but there are question marks.
It’s about having the time but also the right knowledge. Dentists wonder how to discover the relationship between the jawbone and the rest of the skeleton in terms of osteoporosis. What tools and aids are there, says Joanna Golberg.
In a second survey, willingness to pay was also examined among women in the risk group for dentist evaluation for X-rays.
– On average, they were willing to pay 385 SEK for the time it would take a dentist to assess their risk of osteoporosis, says Joanna Golberg.
Warm interest among the surveyed doctors
Another obstacle is the lack of consistent communication methods for healthcare dentists. These items are necessary to prevent patient access between chairs, says Joanna Golberg, who has also studied software that can be used for automatic jaw bone analysis.
Existing but needs development to improve the ability to detect patients at risk.
Perhaps the main issue is the lukewarm interest among clinicians to establish a collaboration. Joanna Golberg also wanted to conduct focus group interviews with general practitioners, but despite repeated attempts, she was unsuccessful in getting one group together. Participate with a medical professional and positively look at the ideas.
– I think the doctors’ skepticism is due to the large workload. Joanna Golberg says they fear the pressure will increase even more.
hypothesis:
Call:
Joanna Gullberg, Faculty of Dentistry, University of Malmö [email protected]

“Extreme tv maven. Beer fanatic. Friendly bacon fan. Communicator. Wannabe travel expert.”










More Stories
What Is a Blue Moon and When Can You See It in the UK?
LHC Achieves Key Milestone in 2026 Physics Programme
Why Rare Earth Metals for Electric Cars Are Crucial for Modern Mobility